Fentanyl vs Tylenol: Clinical Comparison, Potency & Side Effects
Fentanyl and Tylenol sit at opposite ends of the American pain management spectrum. One is a high-potency Schedule II synthetic narcotic, while the other is a non-opioid over-the-counter (OTC) staple.
- Fentanyl: The strongest opioid in medical use, measured in micrograms (mcg).
- Tylenol (Acetaminophen): A versatile analgesic and fever-reducer available without a prescription.
While they are rarely 'alternatives' to each other, understanding how they differ in safety, liver impact, and potency is crucial for U.S. consumer health.
Dr. Kelsey Hopkins, MD
Dr. Hopkins practices rural family medicine in Southern Illinois, with a focus on community healthcare and chronic pain management.
Quick Reference Comparison
| Clinical Feature | Fentanyl | Tylenol |
|---|---|---|
| U.S. Regulation | Schedule II Controlled | OTC (Over-The-Counter) |
| Drug Class | Synthetic Opioid Pure Agonist | Non-aspirin Analgesic / Antipyretic |
| Mechanism | Mu-Opioid Receptor Binding | Central Prostaglandin Inhibition |
| Potency (Relative) | EXTREME (100x Morphine) | MILD (Non-narcotic) |
| Addiction Risk | Very High | None / Negligible |
Clinical Profile: Fentanyl
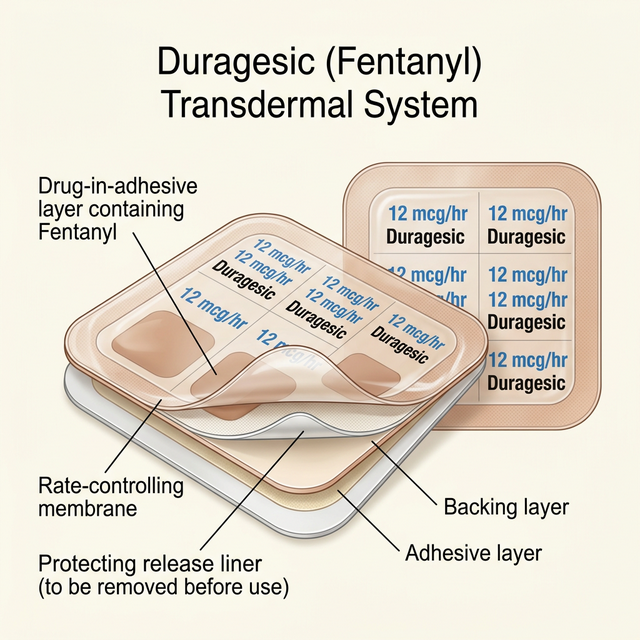
Fentanyl is a specialized tool for chronic or surgical pain within the USA. Its features include:
- Mcg Dosing: Precisely dosed because even a tiny amount can stop breathing.
- Patch Form: Often used as 72-hour skin patches to avoid pills.
- Restricted Access: Requires a strict written prescription by a U.S. clinical specialist.
It is reserved for the most severe pain cases where OTC drugs like Tylenol have no effect.
Clinical Profile: Tylenol

Tylenol is the brand name for Acetaminophen. In the U.S. market, it is valued for:
- Fever Control: One of the world's most effective antipyretics for adults and children.
- Safety Profile: Safe for most people's stomachs, unlike Ibuprofen or Naproxen.
- Accessibility: Available in every pharmacy, grocery store, and convenience store in America.
While it doesn't build dependence, it has a strict safety 'ceiling' to prevent liver damage.
Mechanism of Action: How They Work
How do these molecules interact with pain signals in American patients?
- Fentanyl: Blocks pain in the brain and spinal cord by mimicking natural endorphins on Mu-receptors.
- Tylenol: Acts primarily in the brain to block enzymes that send 'pain signals' up the nerves.
- Inflammation: Neither drug is a powerful anti-inflammatory (unlike Motrin or Advil).
Receptor vs. Chemical Modulation
Opioid Switch
Fentanyl turns off the 'main switch' for pain perception.
Pain Messenger
Tylenol dampens the chemical signals sent to the brain.
Liver Focus
Tylenol's primary breakdown occurs via the NAPQI pathway.
Blood-Brain
Both cross the barrier easily but with different targets.
FDA-Approved vs. Off-Label Uses
FDA oversight and common U.S. clinical use:
- Fentanyl FDA: Management of severe, continuous chronic pain in tolerant patients.
- Tylenol FDA: Temporary relief of minor aches, pains, and reduction of fever.
- Off-Label Tylenol: Sometimes used by doctors to potentiate the effects of opioids (The 'Opioid-Sparing' effect).
Potency and Clinical Strength
Potency comparison (Modern U.S. Standards):
- Fentanyl (Extreme): Thousands of times stronger than Tylenol; they are not comparable in efficiency.
- Tylenol (Mild): Ideal for headaches, toothaches, and minor surgical recovery.
- The Safety Rule: Doubling a dose of Tylenol won't kill you instantly, but doubling Fentanyl usually will.
Bioavailability & Metabolism
- Fentanyl Patch: Slowly seeps into the fat layer via passive diffusion; 92% uptake.
- Tylenol Tablets: Rapidly absorbed by the stomach; 100% uptake within 30-60 minutes.
- Liver Strain: Tylenol puts far more acute stress on hepatic (liver) pathways than Fentanyl.
Half-Life & Duration of Action
- Fentanyl: Lasts 72 hours per application (Patches).
- Tylenol: Lasts 4-6 hours; wears off quickly and requires repeat dosing.
- Consistency: Fentanyl gives 'flat' blood levels; Tylenol creates 'peaks and valleys'.
Clinical Efficacy and Indications
Effectiveness in U.S. patient populations:
- Post-Op: Tylenol is now the #1 first-line choice to avoid opioid addiction after minor surgery in the USA.
- Malignant Pain: Fentanyl is the standard for dignity and comfort in terminal cancer pain.
Typical Dosage and Administration
- Tylenol: 325mg (Regular), 500mg (Extra Strength), 650mg (Extended Relief).
- Fentanyl: 12mcg, 25mcg, 50mcg, 75mcg, 100mcg per hour patches.
- Strict Limit: Tylenol has a HARD maximum of 4,000mg in 24 hours for healthy adults.
Side Effects and Adverse Reactions
Adverse reaction comparison in the United States:
- Stomach: Tylenol is generally 'stomach-safe' compared to aspirin.
- Lungs: Fentanyl is a powerful respiratory depressant (Stops breathing).
- Skin: Fentanyl patches can cause localized rashes or redness.
Comprehensive Side Effect Analysis
| Adverse Event | Fentanyl (Narcotic) | Tylenol (OTC) |
|---|---|---|
| Nausea | Very High | Low |
| Stops Breathing | Extremely High Risk | No Risk |
| Liver Damage | Minimal | High (at overdose) |
| Addiction Potential | Extreme | None |
| Sedation / Fog | Extreme | None |
🔴 Fentanyl Risks
- Severe sedation and sleepiness
- Nausea and vomiting
- Heavy opioid constipation
- Itchy skin (Narcotic itch)
- Confusion in the elderly
🔴 Tylenol Risks
- No common side effects at normal doses
- Rare allergic skin reaction
- Mild dizziness (rare)
- Stomach upset (if taken on empty stomach)
- Sweating
⚠ Critical Safety Note
Serious adverse reactions require immediate medical attention. The following are life-threatening signs:
- Acute Hepatic (Liver) Failure (Tylenol)
- Lethal respiratory arrest (Fentanyl)
- Heat-induced patch overdose
- Severe drug-to-drug interactions
- Coma
Safety, Addiction Risk, and Controlled Status
⚠ U.S. Regulation: FENTANYL: EXTREME | TYLENOL: LOW (AS DIRECTED)
Safety regulations and risks in American healthcare:
- The Hidden Tylenol: Thousands of U.S. OTC cold meds contain Tylenol; accidental overdose is common.
- The Patch Rule: Never fold a Fentanyl patch or let it touch a child's skin.
- Alcohol: Mixing alcohol with Tylenol creates a toxic liver environment almost instantly.
- Never exceed 4,000mg of Acetaminophen per day.
- Always check 'hidden' Tylenol in NyQuil or Percocet.
- Fentanyl: Avoid MRI machines or heating pads with the patch on.
- Keep Naloxone (Narcan) in the house for Fentanyl users.
Pharmacy Cost & U.S. Healthcare Access
- Tylenol: Cent-per-tablet ($5-$10 for a large bottle).
- Fentanyl: Significant cost via prescription ($60-$150).
Clinical Decision Flow: Which Should You Choose?
Clinical decision tree for U.S. consumers:
- Choose Tylenol: For headaches, viral fever, minor sprains, or everyday relief.
- Choose Fentanyl: ONLY if prescribed by a specialist for end-stage chronic pain.
U.S. Pain Management Strategy
Frequently Asked Questions
No. It is a non-opioid, non-aspirin analgesic.
Yes, doctors often combine them for better pain control, as they target different pathways.
When the liver is overwhelmed, it creates a toxic byproduct (NAPQI) that kills liver cells.
Yes, Tylenol has no effect on the bowels, whereas Fentanyl causes severe slowing.
NO. Fentanyl is a highly restricted Schedule II drug; Tylenol is OTC.
