The Science of Central Sensitization
Fibromyalgia is no longer considered a "musculoskeletal" disorder in the United States; it is now classified as a disorder of 'Central Pain Processing.' Imagine the brain's pain volume dial is stuck in the 'max' position. Even gentle pressure or minor stress can trigger a cascade of pain signals that the nervous system fails to filter out correctly. Understanding this neurological basis is the first step toward effective management.
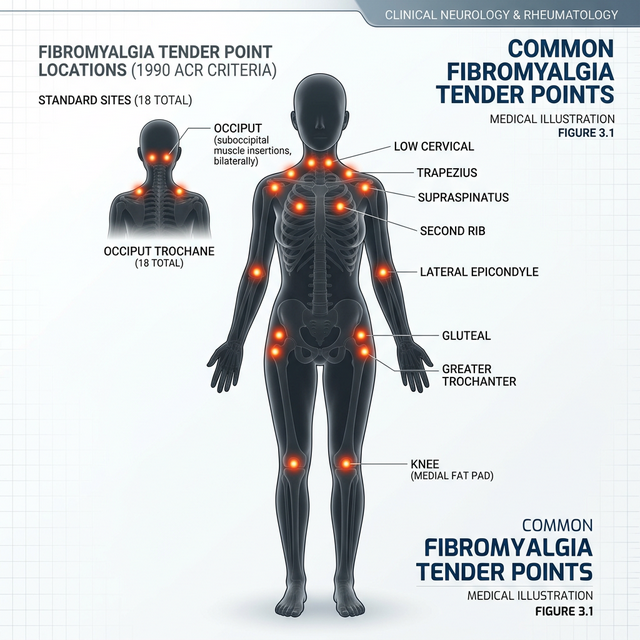
Visualization of the 'Central Sensitization' model, where the spinal cord and brain amplify peripheral signals into widespread pain.
Clinical Management Pathways in the USA
U.S. clinical protocols for Fibromyalgia focus on "Multi-modal" care—combining medications that adjust nerve signaling with behavioral and physical therapies to 'retrain' the brain.
| Medication Class | U.S. Role in Therapy | Common Examples |
|---|---|---|
| SNRIs | Boosts serotonin/norepinephrine to block pain. | Duloxetine (Cymbalta), Milnacipran |
| Gabapentinoids | Reduces excessive nerve electrical firing. | Pregabalin (Lyrica), Gabapentin |
| Tricyclics (Low Dose) | Improves restorative sleep architecture. | Amitriptyline, Cyclobenzaprine |
| CBT/Mindfulness | Reduces the 'emotional' load of chronic pain. | Brain-retraining protocols |
The 'Pacing' Model of Activity
In American rehabilitative medicine, the most common mistake Fibromyalgia patients make is the 'Boom-Bust' cycle—doing too much on a 'good' day and then being bedridden for three. U.S. physical therapists teach 'Pacing,' where patients perform a set amount of activity regardless of how they feel, gradually increasing the baseline without triggering a 'crash' or sympathetic nervous system overload.
Addressing 'Fibro Fog' & Cognitive Health
The cognitive symptoms of Fibromyalgia are often reported as more distressing than the pain itself. U.S. neurologists attribute this to 'Brain Overload'—when the brain is so busy processing pain signals, it lacks the resources for memory and focus. Strategies such as 'Brain Dumping' (writing everything down), prioritizing sleep, and reducing sensory 'clutter' have shown success in American clinical settings in improving clarity and focus.
Frequently Asked Questions (Fibromyalgia)
Is Fibromyalgia a 'real' disease?
Yes. In the United States, Fibromyalgia is clinically recognized as a disorder of 'Central Sensitivity,' where the brain and spinal cord process pain signals more intensely than normal.
What are the common symptoms beyond pain?
Symptoms often include 'Fibro Fog' (cognitive difficulties), debilitating fatigue, non-restorative sleep, and heightened sensitivity to lights, sounds, and smells.
Are opioids effective for Fibromyalgia?
Generally, no. U.S. clinical boards advise against long-term opioid use for Fibromyalgia, as they may actually worsen the 'Central Sensitization' through a process called Opioid-Induced Hyperalgesia.
Which medications are FDA-approved for it?
Currently, three medications are FDA-approved in the U.S.: <Link href="/medications/pregabalin">Pregabalin (Lyrica)</Link>, <Link href="/medications/duloxetine">Duloxetine (Cymbalta)</Link>, and <Link href="/medications/milnacipran">Milnacipran (Savella)</Link>.
Is there a specific test for Fibromyalgia?
No. It is a 'Clinical Diagnosis.' Doctors in the U.S. use the Widespread Pain Index (WPI) and Symptom Severity (SS) scale, along with ruling out other conditions like Lupus or RA.
What type of exercise is recommended?
U.S. specialists recommend 'Graded Exercise Therapy' (GET), starting with extremely low-impact movement like warm-water aerobics or gentle walking, to avoid 'flaring' the nervous system.
How does sleep affect the pain?
Sleep is the #1 priority in Fibromyalgia management. Lack of deep 'Stage 4' sleep prevents the body from suppressing pain signals, leading to higher pain scores the following day.
Does Fibromyalgia cause tissue damage?
No. Unlike Arthritis, Fibromyalgia does not cause physical damage to your joints or muscles. It is a functional disorder of the 'wiring' (nervous system), not the 'hardware' (tissues).
Can diet help manage symptoms?
Many patients in the U.S. benefit from avoiding excitotoxins like MSG and artificial sweeteners, and focusing on a nutrient-dense, whole-food diet to reduce overall systemic stress.
Is Fibromyalgia permanent?
While currently considered chronic, many U.S. patients reach a state of functional remission where symptoms are manageable and do not prevent a full, active life.
Clinical References
- Mayo Clinic. (2025). Fibromyalgia Diagnosis and Treatment Roadmap.
- The American College of Rheumatology. (2024). Revised Criteria for Fibromyalgia.
- Journal of Pain Research. (2026). Neuroimaging and Central Sensitization.