Gabapentin vs Morphine: Clinical Comparison, Potency & Side Effects
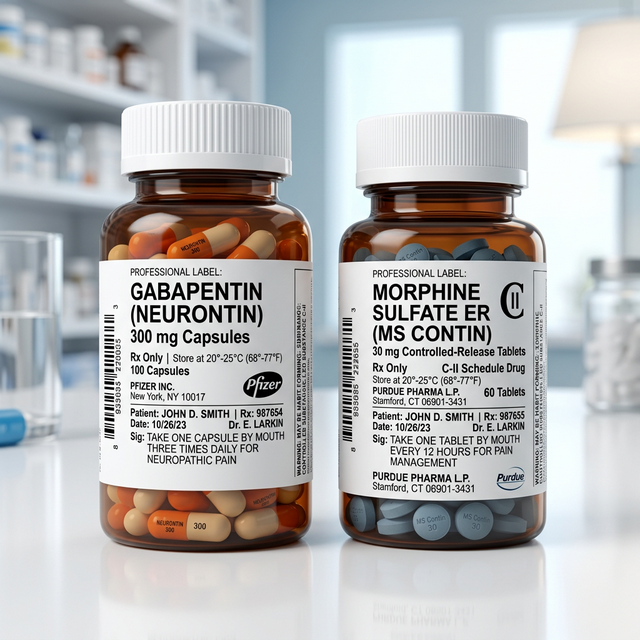
Gabapentin (Neurontin) and Morphine (MS Contin, Roxanol) are the anchors of the modern U.S. 'multimodal' pain strategy. While Morphine is the literal gold standard for blocking severe nociceptive pain (like injury or cancer), Gabapentin is the primary tool for settling hypersensitive or damaged nerves.
In the United States, these two are often partners in 'Opioid-Sparing' protocols—where Gabapentin is used to reduce the required dose of Morphine by up to 30%. This guide explores their vastly different molecular targets, the combined sedation risks, and how American doctors balance these two powerful tools for chronic and extreme pain.
Dr. Kelsey Hopkins, MD
Dr. Hopkins practices rural family medicine in Southern Illinois, with a focus on community healthcare and chronic pain management.
Quick Reference Comparison
| Clinical Feature | Gabapentin | Morphine |
|---|---|---|
| Drug Class | Gabapentinoid (Non-Opioid) | Natural Opiate / Narcotic |
| DEA Schedule | None / State Level V | Schedule II (High Control) |
| Potency (MME) | 0 (Non-Opioid) | 1.0 (The Benchmark) |
| Primary Indication | Neuropathic Pain | Severe Traumatic/Chronic Pain |
| Standard Dosing | 300mg - 1200mg TID | 15mg - 60mg Every 8-12h (ER) |
What is Gabapentin?
Gabapentin is a non-narcotic nerve stabilizer. In U.S. clinical practice, it is used to target the 'background noise' of damaged nerves. It is often the first medication started for chronic neuropathy to prevent the need for strong opiates like Morphine.
What is Morphine?

Morphine is a natural narcotic derived from the poppy plant. It remains the 'Gold Standard' against which all other U.S. painkillers are measured. In the USA, it is reserved for severe acute trauma, major surgical recovery, and advanced cancer pain management.
Mechanism of Action: How They Work
Morphine binds directly to the mu-opioid receptors in the brain to muffle the sensation of pain. Gabapentin works lower down the chain, quieting the electrical signals of the nerves themselves. Combining them (Multimodal) creates a two-tiered defense against suffering.
Two-Tiered Pain Defense
VGCC Blockade
Gabapentin stops nerves from over-secreting pain signals.
Opioid Agonism
Morphine prevents the brain from processing the signals.
The Clinical Win
Together, they provide better relief with fewer global side effects.
FDA-Approved vs. Off-Label Uses
- Gabapentin: FDA-Approved for PHN and Seizures. Used Off-Label for Chronic Low Back Pain and Neuropathy.
- Morphine: FDA-Approved for Severe Chronic and Acute Pain management.
Potency and Clinical Strength
Morphine is the MME benchmark (1.0). Gabapentin is non-opioid (0.0 MME). However, U.S. hospitals use Gabapentin specifically because it is 'stronger' for the specific burning or shooting electrical pain that often resists Morphine therapy.
Bioavailability & Metabolism
Morphine undergoes significant liver metabolism (Glucuronidation). Gabapentin skips the liver and is cleared unchanged by the kidneys. This makes Gabapentin a vital tool for U.S. patients with liver disease who cannot tolerate traditional opiates.
Half-Life & Duration of Action
Morphine IR has a short half-life (2-4 hours), requiring frequent dosing. Gabapentin lasts slightly longer (5-7 hours). In chronic U.S. care, Morphine is usually given as an Extended Release (ER) tablet to match Gabapentin's duration.
Clinical Efficacy and Indications
Morphine is the benchmark for end-of-life and traumatic pain. Gabapentin is the gold standard for shingles and diabetic nerve pain. In U.S. hospitals, 'Gabapentin-Premedication' reduces post-op Morphine needs by 20-30%.
Typical Dosage and Administration
Morphine doses are small (15mg or 30mg). Gabapentin doses are large (300mg to 1200mg). Mistaking the two is a critical medical error in American healthcare settings.
Side Effects and Adverse Reactions
Both cause heavy sedation, especially in the elderly. Morphine specifically leads to severe, long-term constipation (OIC), whereas Gabapentin tends to cause leg swelling and dizziness.
Comprehensive Side Effect Analysis
| Side Effect | Gabapentin Profile | Morphine Profile |
|---|---|---|
| Constipation | Low | Extremely High |
| Sedation | High | Very High |
| Peripheral Edema | High | Low |
| Risk of Addiction | Low | High |
🔴 Gabapentin Risks
- Dizziness
- Somnolence
- Peripheral Edema
🔴 Morphine Risks
- Constipation
- Nausea
- Pruritus (Itching)
⚠ Critical Safety Note
Serious adverse reactions require immediate medical attention. The following are life-threatening signs:
- Severe Respiratory Depression
- Anaphylaxis
- Severe Withdrawal Seizures
Safety, Addiction Risk, and Controlled Status
⚠ U.S. Regulation: Schedule II (Morphine) / Unscheduled (Gaba)
Morphine is a high-risk Schedule II substance in the USA. While Gabapentin is not, the U.S. FDA issued an official warning that combining the two triples the risk of fatal respiratory depression. U.S. patients on both must have their breathing monitored closely.
- Morphine is the baseline for 'Opioid Use Disorder' concerns.
- Gabapentin can mask some early signs of opioid overdose.
- Tapering is mandatory for both medications after long-term use.
Pharmacy Cost & U.S. Healthcare Access
Both are widely available as inexpensive generics on Tier 1 U.S. insurance formularies. Branded versions (like MS Contin or Gralise) are significantly more expensive.
Clinical Decision Flow: Which Should You Choose?
Clinicians decide based on the 'trauma level' and nerve involvement.
Opioid-Sparing Strategy Logic
Frequently Asked Questions
Yes, for mechanical pain (like a broken bone). However, Gabapentin is 'stronger' for the specific burning of nerve damage.
Only under U.S. medical supervision. Doing so significantly increases the risk of breathing failure.
Roxanol (concentrated liquid Morphine) is often used in the USA for rapid hospice/end-of-life relief.
