Hydrocodone vs Codeine: Clinical Comparison, Potency & Side Effects
Dr. Kelsey Hopkins, MD
Dr. Hopkins practices rural family medicine in Southern Illinois, with a focus on community healthcare and chronic pain management.
Quick Reference Comparison
| Clinical Feature | Hydrocodone | Codeine |
|---|---|---|
| Drug Class | Semi-synthetic Opioid | Natural Opium Alkaloid |
| Potency (to Morphine) | 1x (Equianalgesic) | 0.15x (Much Weaker) |
| Metabolic Pathway | CYP2D6 / CYP3A4 | CYP2D6 (Prodrug) |
| Typical Combo | Acetaminophen (Norco) | Acetaminophen (Tylenol #3) |
| DEA Schedule | Schedule II | Schedule III (Tylenol #3) |
| Primary Use | Moderate-Severe Pain | Mild-Moderate Pain / Cough |
| Side Effect Risk | High (Sedation/GI) | Moderate (High Nausea) |
What is Hydrocodone?

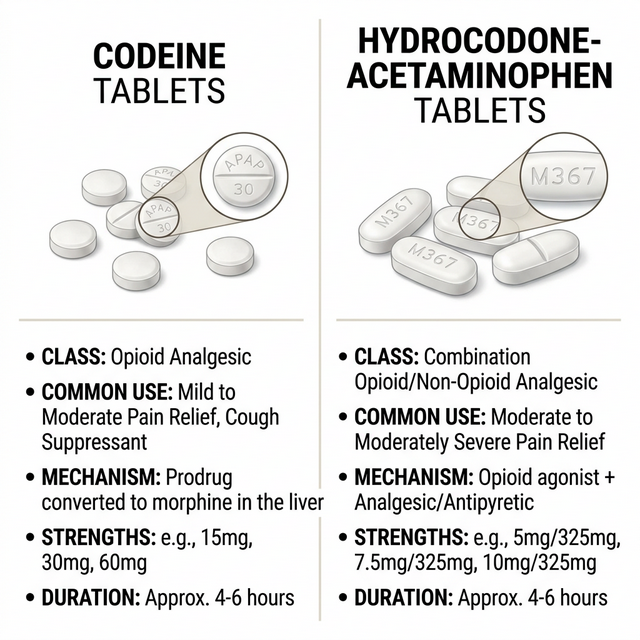
Hydrocodone is a semi-synthetic opioid derived from codeine or thebaine. In the United States, it is most commonly found in combination with acetaminophen (Tylenol) under brand names like Norco, Vicodin, and Lortab. For years, Hydrocodone was the most frequently prescribed medication in the entire USA, becoming the standard for dental surgery recovery, moderate injury management, and chronic back pain. It works by binding to mu-opioid receptors in the brain, altering how the body perceives and responds to pain. In 2014, the U.S. DEA reclassified all hydrocodone products from Schedule III to Schedule II due to their high potential for abuse and addiction.
The role of Hydrocodone in the USA is for moderate-to-moderately-severe pain. Unlike Codeine, Hydrocodone is an 'active' drug, meaning it doesn't rely entirely on the body's metabolism to work. This makes it much more predictable than codeine in the American population. While it is equianalgesic to oral morphine (1mg Hydrocodone = 1mg Morphine), it is perceived by many U.S. clinicians as being better tolerated with slightly less itching and digestive distress than natural opiates. It is also available in extended-release forms (Zohydro, Hysingla) for 24-hour management of severe chronic pain.
Clinically, Hydrocodone is the 'Step 2' on the WHO pain ladder in the USA. If a patient is failing on maximized doses of Ibuprofen and Tylenol, a combination of Hydrocodone and Acetaminophen is usually the next logical clinical transition. Its widespread availability and familiarity among U.S. practitioners make it a cornerstone of post-surgical outpatient care.
What is Codeine?

Codeine is a natural alkaloid found in the opium poppy. In the American medical hierarchy, Codeine is considered a 'weak' opioid or a 'prodrug'. This means that Codeine itself has almost no pain-killing effect; instead, the body must convert it into morphine using the liver enzyme CYP2D6. If an American patient lacks this enzyme (about 10% of the population), Codeine will do absolutely nothing for their pain. Conversely, 'ultra-rapid metabolizers' can convert it into morphine too quickly, leading to dangerous and potentially lethal toxicity, even at 'normal' doses. This variability has led many U.S. pediatric hospitals to ban the use of codeine entirely.
In the USA, Codeine is most commonly found in 'Tylenol with Codeine #3', which contains 30mg of codeine and 300mg of acetaminophen. It is also a powerful antitussive (cough suppressant) found in many prescription-strength cough syrups. Because it is chemically 'milder' than Hydrocodone, Codeine combinations (with less than 90mg per dose) are classified as Schedule III in the USA, meaning they are slightly less regulated than the Schedule II Hydrocodone and can sometimes allow for limited refills.
Despite its long history, Codeine is falling out of favor in modern U.S. evidence-based medicine. The high rate of nausea, the intense constipation, and the metabolic unpredictability make it a second-choice drug behind more reliable options like low-dose Hydrocodone or even high-dose NSAIDs for many American doctors.
Mechanism of Action: How They Work
Hydrocodone acts primarily as an agonist at the mu-opioid receptor, actively binding to provide immediate relief. Codeine is uniquely a prodrug that must be converted into morphine via the CYP2D6 enzyme in the liver before it can effectively bind to receptors and alleviate pain.
Receptor Dynamics
Direct Binding
Hydrocodone actively binds to receptors.
Prodrug Conversion
Codeine relies on liver enzymes to work.
Histamine Trigger
Codeine releases high levels of body histamine.
FDA-Approved vs. Off-Label Uses
- Hydrocodone: FDA-Approved for severe pain requiring an opioid analgesic and for which alternative treatments are inadequate.
- Codeine: FDA-Approved for mild-to-moderate pain and as an antitussive (cough suppressant).
Potency and Clinical Strength
The strength comparison between Hydrocodone and Codeine is a gap of nearly 6 to 1. In the USA, 30mg of Codeine (the amount in a Tylenol #3) is roughly equivalent to just 4.5mg of Morphine. Since Hydrocodone is equianalgesic with Morphine, Hydrocodone is approximately 6 times stronger than Codeine milligram-for-milligram. For a U.S. patient who has been on Codeine and is not achieving relief, switching to a 5mg Norco (Hydrocodone) represents a significant increase in analgesic power.
Bioavailability & Metabolism
Codeine relies completely on CYP2D6 for conversion. Up to 10% of patients lack this enzyme, experiencing no relief, while ultra-rapid metabolizers risk toxic overdose. Hydrocodone is active on its own and provides consistent relief independent of rapid metabolic variations, although it uses CYP3A4 for clearance.
Half-Life & Duration of Action
Both medications have an active half-life of roughly 3 to 4 hours in their immediate-release forms (which typically include acetaminophen). Dosing is standard at every 4 to 6 hours for continuous pain control.
Clinical Efficacy and Indications
Effectiveness data in the USA shows Hydrocodone is superior for postsurgical recovery and orthopedic trauma. Its higher potency and direct action make it more reliable for managing the intense pain of a bone fracture or a dental extraction. Codeine's primary 'win' is in Cough Suppression. Many U.S. physicians still view Codeine as the gold standard for a 'unrelenting, non-productive cough' that keeps a patient from sleeping.
Typical Dosage and Administration
Hydrocodone dosing in the USA typically starts at 5mg (combined with 325mg of Tylenol) every 4 to 6 hours. The most common U.S. dosages are 5/325mg, 7.5/325mg, and 10/325mg. Because it is Schedule II, a new secure script is required for every fill, and refills are strictly forbidden in all 50 states. For chronic relief, U.S. patients may use pure Hydrocodone ER (Hysingla) in doses up to 120mg once daily.
Codeine dosing typically starts at 30mg to 60mg every 4 hours. The U.S. maximum daily dose is traditionally 360mg. As a Schedule III substance in combination forms, U.S. doctors can technically write for up to 5 refills within a 6-month period, although internal clinic policies in the USA are increasingly restricting this to match the stricter Schedule II protocols.
Both medications carry the risk of Acetaminophen Toxicity since they are almost always prescribed as combination pills. U.S. patients must be strictly monitored to ensure they do not exceed 4,000mg of Tylenol per day from all sources, a common error that leads to liver failure in the United States.
Side Effects and Adverse Reactions
Both medications carry significant side effect profiles typical of opioids, including constipation, dry mouth, and the risk of respiratory depression.
Comprehensive Side Effect Analysis
| Adverse Event | Hydrocodone (Norco) | Codeine (Tylenol #3) |
|---|---|---|
| Nausea / Vomiting | Moderate | High / Very High |
| Constipation | Severe | Very Severe |
| Itching (Pruritus) | Moderate | High (Histamine release) |
| Sedation / Fog | Moderate / High | Moderate |
| Dry Mouth | High | High |
| Metabolic Failure Risk | Low | High (CYP2D6 variability) |
🔴 Hydrocodone Risks
- Moderate Opioid-Induced Constipation
- Dizziness and Vertigo
- Nausea and Stomach Cramps
- Dry Mouth (Xerostomia)
- Drowsiness and Sleepiness
🔴 Codeine Risks
- Severe Digestive Distress / Nausea
- Intense Itching and Facial Flushing
- Severe Constipation
- Significant Dry Mouth
- Dizziness and Lightheadedness
⚠ Critical Safety Note
Serious adverse reactions require immediate medical attention. The following are life-threatening signs:
- Lethal Respiratory Depression
- Acute Liver Failure (from Acetaminophen)
- Lethal Interaction with Alcohol
- Serotonin Syndrome (rare)
- Morphine Toxicity (in Codeine Ultra-Rapid Metabolizers)
Safety, Addiction Risk, and Controlled Status
⚠ U.S. Regulation: NARCOTIC: HIGH / TOXICITY: LIVER-DEPENDENT
The Addiction Risk for both is significant, though Hydrocodone is more frequently a drug of abuse in the USA due to its higher 'spark' and availability. It creates a chemical high that can rapidly lead to dependency. Codeine is also addictive but is often perceived (wrongly) as 'safer' by U.S. patients, which can lead to a dangerous false sense of security.
From a Safety standpoint, the 'Standard of Care' in the USA has shifted away from Codeine because of its Genomic Unpredictability. A child or elderly person in the USA could stop breathing after a single 'normal' dose of codeine if they are an ultra-rapid metabolizer. Hydrocodone, being a Schedule II substance, requires much higher levels of monitoring, including mandatory PDMP checks in almost all U.S. states before a pharmacist can dispense it.
- Hydrocodone is ~6x more potent than Codeine in the USA.
- Codeine is a prodrug; Hydrocodone is an active medication.
- Codeine combination pills are Schedule III; Hydrocodone is Schedule II.
- Both carry a high risk of lethal liver damage if mixed with extra Tylenol.
Pharmacy Cost & U.S. Healthcare Access
Cost is generally low for both as generics in the USA. A standard 30-day supply of generic Norco (Hydrocodone/APAP) or Tylenol #3 (Codeine/APAP) typically costs $15 to $30 at American retail pharmacies. Most U.S. insurance plans (Medicare Part D, Blue Cross, etc.) cover both as Tier 1 generics. However, because of the extra DEA paperwork for Schedule II drugs, some U.S. mail-order pharmacies cannot carry Hydrocodone, making Codeine slightly easier to access for some uninsured U.S. patients.
Clinical Decision Flow: Which Should You Choose?
A U.S. doctor’s choice is driven by Reliability. Most American surgeons will choose Hydrocodone over Codeine because they know it will work for nearly all their patients. Codeine's 10% metabolic failure rate is too high for post-surgical care. However, Codeine remains a standard for treating severe, painful coughs.
Hydrocodone is the reliable, potent workhorse for moderate-to-severe pain in the USA. Codeine is a milder, natural opiate historically used for minor relief and coughs, but it's increasingly sidelined by its own unpredictability.
U.S. Clinical Selection Protocol
Frequently Asked Questions
Yes. Milligram-for-milligram, Hydrocodone is approximately 6 times more powerful than Codeine in U.S. clinical benchmarks.
Codeine or natural opiates cause a significant release of histamine in the body, leading to itching and flushing for many U.S. patients.
It depends. They are chemically related. You must consult your U.S. doctor or allergist before switching.
Because 'ultra-rapid metabolizers' can convert codeine into lethal amounts of morphine too quickly, causing respiratory arrest.
No. Norco contains Hydrocodone and Acetaminophen. It is more potent than Codeine combinations.
Codeine is the traditional gold standard for cough suppression, though Hydrocodone is also used for severe cases in the USA.
No. Both cause significant impairment, drowsiness, and slowed reaction times, making driving dangerous and illegal in the USA.
Both are high-risk, but Codeine is famously notorious for causing some of the most severe opioid-induced constipation.
Yes. Naloxone (Narcan) reverses the respiratory depression caused by both Hydrocodone and Codeine.
Caution is required. Most Hydrocodone and Codeine in the USA already contains 325mg of Tylenol. Adding more can lead to liver failure.
