Gabapentin vs Codeine: Clinical Comparison, Potency & Side Effects
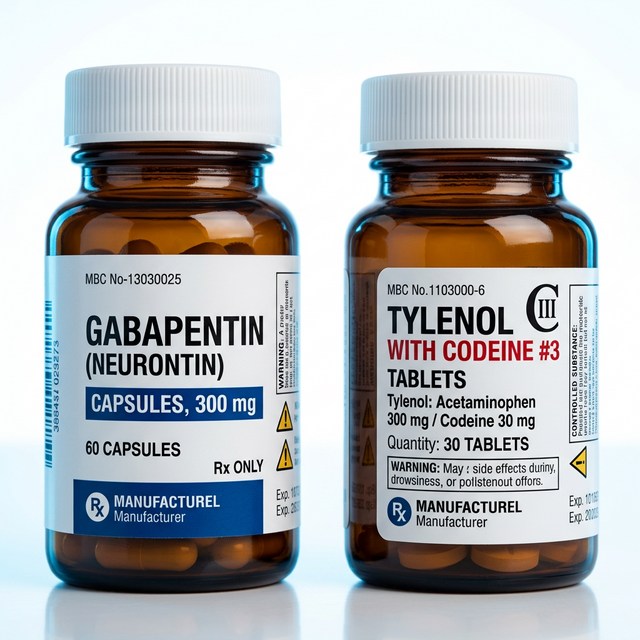
Gabapentin and Codeine treat two fundamentally different types of pain. One is a nerve-specific stabilizer, while the other is a traditional 'bottom-tier' opioid used for acute injuries.
In the United States, there is a growing trend to use Gabapentin as a safer, non-addictive alternative to Codeine for chronic musculoskeletal and neuropathic conditions. This guide compares their different biological targets, the metabolic risks of Codeine (the 'CYP2D6 Lottery'), and why Gabapentin has become a cornerstone of long-term 'nerve calming' therapy in the USA.
Dr. Kelsey Hopkins, MD
Dr. Hopkins practices rural family medicine in Southern Illinois, with a focus on community healthcare and chronic pain management.
Quick Reference Comparison
| Clinical Feature | Gabapentin | Codeine |
|---|---|---|
| Drug Class | Nerve Agent (Gabapentinoid) | Natural Opiate / Narcotic |
| DEA Schedule | Unscheduled / State Level V | Schedule III (Combo) |
| Primary Target | Nerve Calcium Channels | Mu-Opioid Receptors |
| Metabolism | Renal (Kidneys) | Liver (CYP2D6 into Morphine) |
| Standard Dosing | 300mg - 1200mg TID | 30mg - 60mg Every 4-6h |
What is Gabapentin?
Gabapentin is a non-narcotic medication that specializes in quieting 'noisy' nerves. In the USA, it is the gold standard for Postherpetic Neuralgia (Shingles pain) and is increasingly used for chronic back pain where nerves are compressed or damaged.
What is Codeine?

Codeine is a naturally occurring alkaloid from the poppy plant, widely used in the U.S. for mild-to-moderate pain. Key details:
Mechanism of Action: How They Work
Gabapentin works immediately on the calcium channels of nerves to stop pain signal propagation. Codeine is a 'prodrug,' meaning it has almost no pain-relieving effect until the liver converts it into Morphine. This fundamental difference makes Gabapentin more predictable for many U.S. patients.
Nerve vs. Receptor Pathways
VGCC Block
Gabapentin quiets the electrical background of nerves.
Liver Conversion
Codeine requires the CYP2D6 enzyme to become Morphine.
Opioid Target
The converted Morphine blocks central pain switches.
FDA-Approved vs. Off-Label Uses
- Gabapentin FDA: Post-herpetic Neuralgia and focal seizures.
- Codeine Digestion: Must be converted by the liver (CYP2D6) into Morphine to work; roughly 10% of people have a 'genetic block' that makes Codeine useless.
Potency and Clinical Strength
Codeine is the weakest of the U.S. narcotics (0.15 MME). Gabapentin is non-narcotic but is significantly stronger specifically for nerve-driven burning or shocking sensations that Codeine often misses.
Bioavailability & Metabolism
The 'CYP2D6 Lottery' is a major safety concern for Codeine in the USA. About 10% of Americans cannot convert Codeine to Morphine (it won't work), while 'Ultra-Fast' converters may get too much Morphine too quickly. Gabapentin has no such lottery; it is cleared by the kidneys unchanged.
Half-Life & Duration of Action
Codeine has a very short duration of action (2.5 - 4 hours). Gabapentin lasts slightly longer (5-7 hours). For chronic management, Gabapentin provides more stable 'background' control compared to Codeine's peaks and valleys.
Clinical Efficacy and Indications
Codeine is better for short-term dental recovery. Gabapentin is superior for long-term nerve damage. U.S. doctors are increasingly substituting Gabapentin for Codeine in chronic treatment plans to reduce opioid exposure.
Typical Dosage and Administration
Codeine doses are typically 30-60mg per tablet. Gabapentin doses range from 300mg to 1200mg per dose. Both require titration to manage early-stage drowsiness.
Side Effects and Adverse Reactions
Both are central nervous system depressants that cause significant drowsiness. Codeine is notorious for causing intense constipation and nausea in the U.S. patient population.
Comprehensive Side Effect Analysis
| Side Effect | Gabapentin Profile | Codeine Profile |
|---|---|---|
| Drowsiness | High | High |
| Constipation | Low | Very High |
| Nausea/Itching | Rare | High |
| Leg Swelling | High | Rare |
🔴 Gabapentin Risks
- Dizziness
- Unsteadiness
- Peripheral Edema (Swelling)
🔴 Codeine Risks
- Constipation
- Itching/Rash
- Nausea/Sedation
⚠ Critical Safety Note
Serious adverse reactions require immediate medical attention. The following are life-threatening signs:
- Severe Respiratory Suppression
- Genetic Toxicity (Ultra-metabolizers)
- Severe Withdrawal Symptoms
Safety, Addiction Risk, and Controlled Status
⚠ U.S. Regulation: Schedule III/V vs. Unscheduled
Codeine is a narcotic with real potential for dependence and withdrawal. While Gabapentin is not a federal controlled substance, it is increasingly monitored in the USA. Mixing these agents greatly increases the risk of breathing problems, a major focus of U.S. patient safety alerts.
- Codeine has high genetic variability in response.
- Gabapentin is the preferred non-addictive nerve agent.
- Both medications can impair your ability to drive or operate machinery.
Pharmacy Cost & U.S. Healthcare Access
Both are extremely inexpensive generics. Codeine combinations (like Tylenol #3) are among the cheapest prescription narcotics in American pharmacies.
Clinical Decision Flow: Which Should You Choose?
U.S. surgeons decide based on the duration and type of the pain.
Nerve vs. Minor Opiate Decision
Frequently Asked Questions
No. Unlike Codeine (in Tylenol 3), Gabapentin is a non-narcotic that targets nerve pathways rather than opioid receptors.
It has zero risk of opioid addiction and provides more consistent relief without the 'up and down' effect of Codeine.
Generally yes, as they are completely different chemical classes, but always consult a U.S.-licensed provider first.
